Author

NXP
At NXP, innovation is always now, but our focus is always the future. Our dedicated team of experts is united by a passion to make everyday life more remarkable through technologies that continually redefine life as we know it.
The role of technical disruptions in the healthcare industries has been a litany of cautionary tales. Attempts by Theranos to dramatically lower the cost of blood tests created news cycles of the lack of readiness of new technology. The inaccuracies of wearable monitors generated many articles of debates and even ridicules of their usefulness. But these discussions are incomplete without also understanding how new technologies can be used to advance healthcare.
Healthcare is in essence a clinical exercise aided by statistics and technology. Using calibrated and certified medical diagnostic equipment under the supervision of trained professionals; physicians call upon very accurate snapshots of their patients to help confirm their diagnoses. But there is often little quantified information available on the history of a patient, especially at the early stages of an illness and snapshots alone cannot capture the symptoms without considerable uncertainty.
Of course medicine tries to improve on the odds. Patients are classified by sex, age, race, weight, self-reported life styles and family medical histories to reduce the variance of the relevant population. Doctors order a battery of tests to get multiple snapshots of the patient. But in the end, the most accurate snapshots are not enough to overcome variations among the population and diagnoses become inconclusive until later stages.
Personal health monitors can add a dimension of precision and context. A hemoglobin A1C test provides the average level of glucose in a patient over three months. However, a patient experiencing significantly high and low glucose levels could present a seemingly normal average. A continuously worn health monitor captures how a health parameter for a patient has changed, and the rate of that change: information that would be spotty and expensive to collect in a clinical setting.
Medical practitioners often voice concerns over the accuracy of consumer wearable gadgets. The upgrade from novelty gadgets to reliable health monitors requires progress in the following areas:
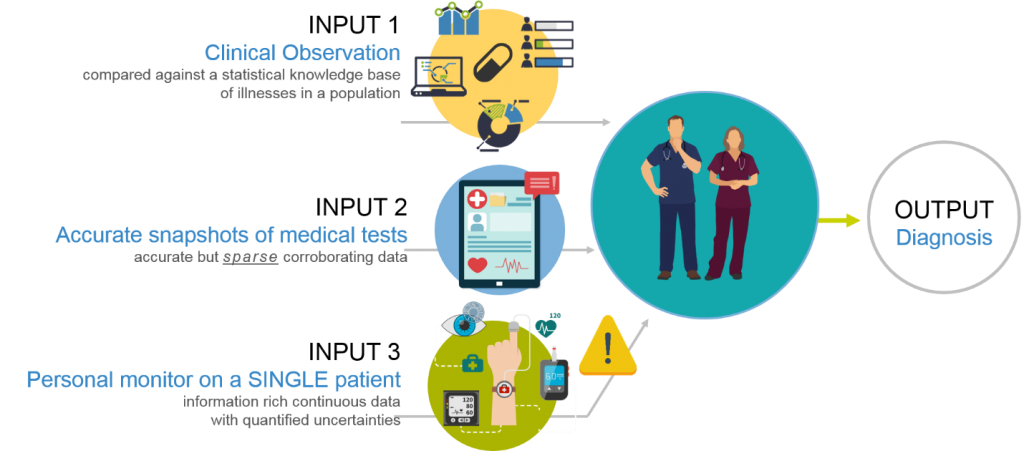
Aligning all the necessary changes may amount to a paradigm shift from conventional “sickcare” to precision (or personalized) healthcare and will require advances in sensing technologies, algorithms, machine learning techniques, security and privacy protocols and medical practices. But it is a change for the better, and long overdue.

At NXP, innovation is always now, but our focus is always the future. Our dedicated team of experts is united by a passion to make everyday life more remarkable through technologies that continually redefine life as we know it.

June 26, 2019

March 6, 2020
by Steven Thoen